2024 • At-Bay • Product Design Lead
AI-powered cybersecurity claims intake automation
Role
Defined the AI rollout strategy and designed intake and verification workflows for FNOL automation — shaping how the claims org introduced AI extraction into a high-stakes environment while maintaining decision quality and compliance.
Outcome
Intake time reduced from 20+ minutes to under 5
98% extraction accuracy on policy ID and insured name
86% accuracy on segmentation (phase two) — remaining cases route to human review, feeding corrections back into the model
Cleared intake backlog and established a scalable process that kept pace with growing claim volume
Team / Stakeholders
Product Manager
Engineering (Tel Aviv)
Claims Team (Operations, Adjusters, Managers)
An AI-powered intake system that extracts policy data from broker emails, populates claim fields automatically, and routes new claims through a structured verification and assignment workflow — replacing a fully manual cross-referencing process.
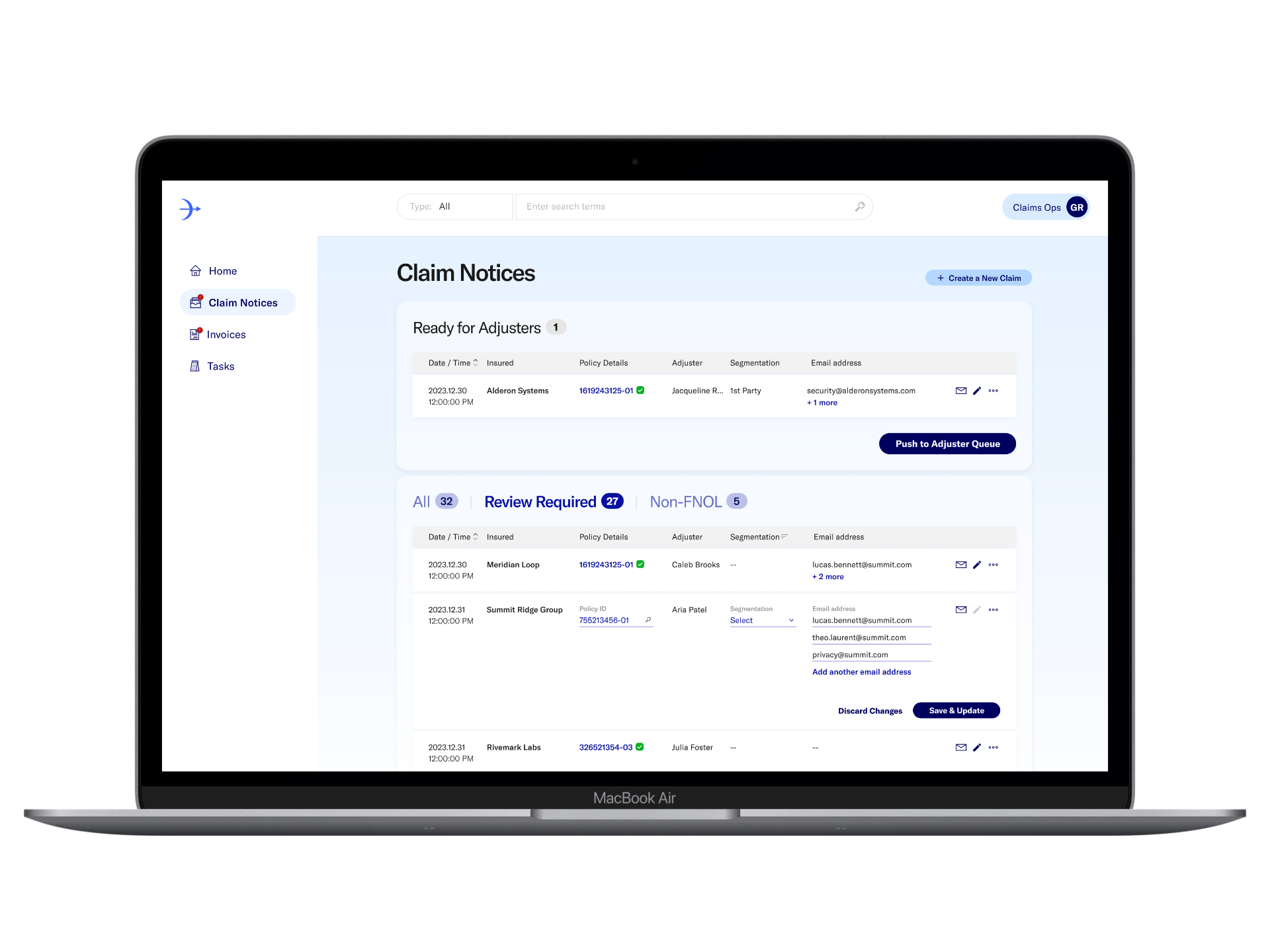
The Challenge
When a new claim came in, claim ops had to manually cross-reference policy data in a separate system, enter every field by hand into a tracking spreadsheet, and send acknowledgment emails individually.
A single claims intake took 5–30 minutes depending on complexity, across a caseload of 150+ open claims per adjuster.
Key Decisions
Risk-based AI rollout behind feature flag
Rather than extracting everything at once, I constrained phase one to the lowest-risk fields — policy ID and insured name. Phase two expanded to segmentation and email addresses only after the model proved itself. Slower rollout, but it built trust without introducing risk.
Intentional friction in verification
I added extra confirmation steps to prevent auto-pilot errors. In claims, a wrong policy number creates real downstream problems — so I optimized for decision quality over speed.
Evolved role-based access post-launch
At MVP, all roles had access to the full FNOL queue to clear a backlog. Once the backlog cleared, I refined access — managers assign, claim ops verify, adjusters see only a "pending claims" filter. The roles weren't assumed upfront; they were shaped by observed usage.
Compliance-aware acknowledgment logic
Acknowledgment emails are legally required — but for ransomware claims, notifying the wrong contact could tip off an attacker. I separated obligation from execution: standard claims auto-send at creation, ransomware claims suppress communication and create a structured human task instead.
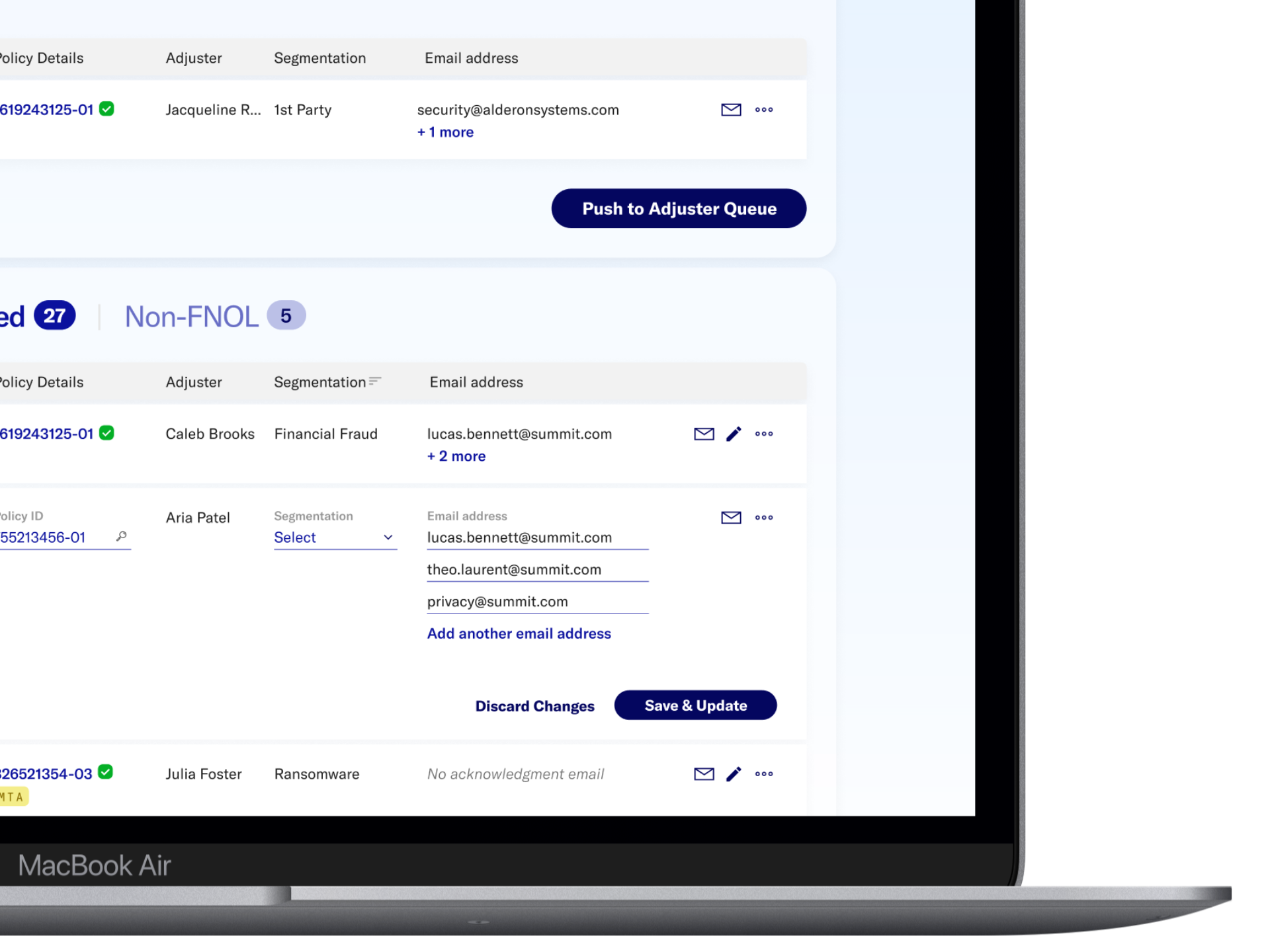
What informed my decisions
Conversations with adjusters and claim ops showed that the bottleneck wasn't just data entry — it was the context-switching between systems that made intake so draining. I mapped the full extraction pipeline, verification checkpoints, failure states, and role-based routing before touching any UI — which revealed that access rules and acknowledgment logic needed to be claim-type-aware, not one-size-fits-all.
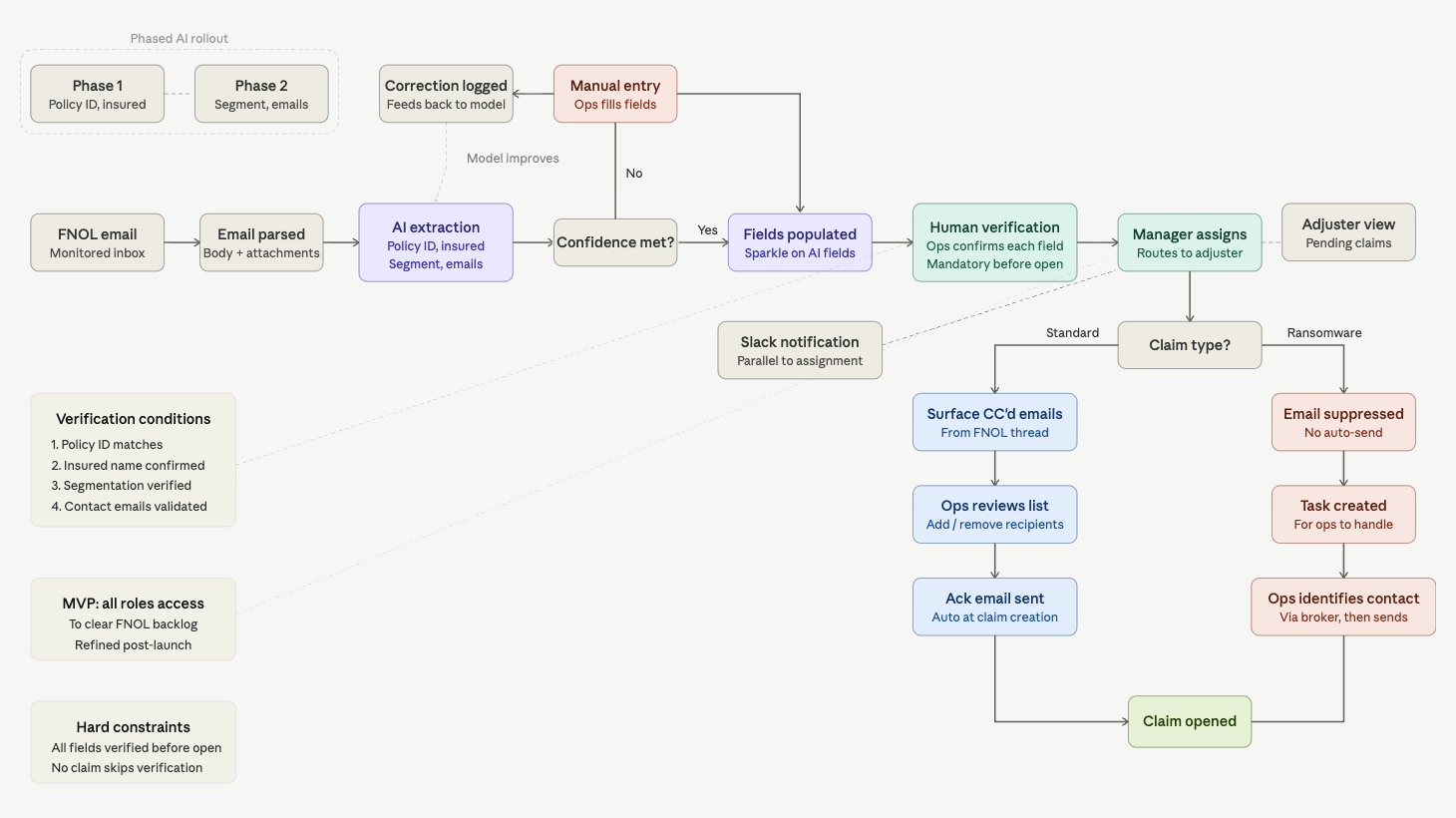
Sample mapping of FNOL automation flow (actual version not shown for compliance reasons)
Results
Intake time reduced from 20+ minutes to under 5
98% extraction accuracy on policy ID and insured name
86% accuracy on segmentation (phase two) — remaining cases route to human review, feeding corrections back into the model
Cleared intake backlog and established a scalable process that kept pace with growing claim volume
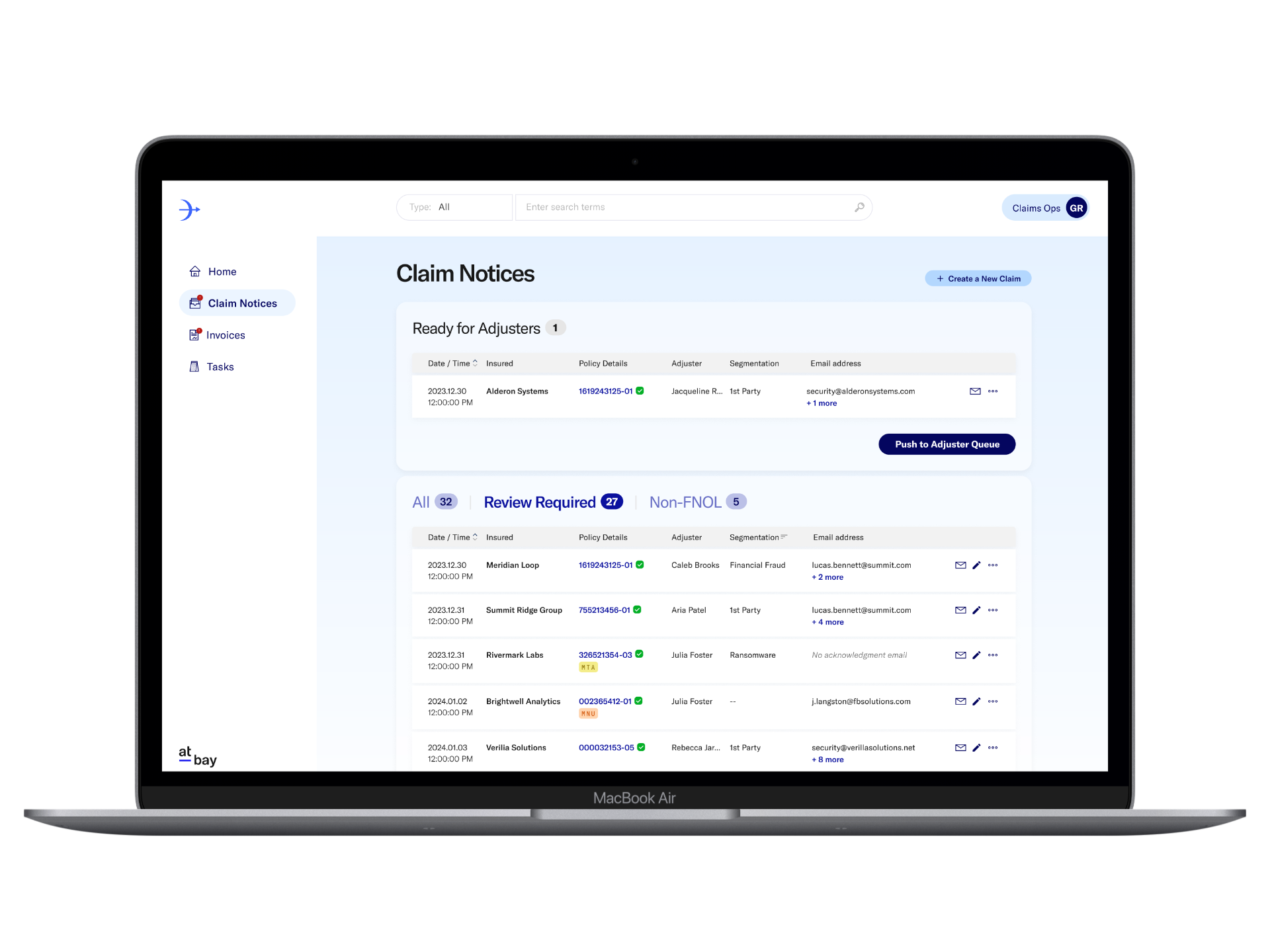
View other projects
AI-powered transcription for broker meetings
Customer-facing death claims intake & profile experience

